Metformin Risk & Suitability Checker
Personal Health Profile
Select the options that apply to your current health status.
Disclaimer: This tool is for educational purposes only and does not constitute medical advice. Always consult your healthcare provider before starting or stopping any medication.
Metformin is the most prescribed medication for type 2 diabetes in the world. It works well, it’s cheap, and doctors trust it. But you’ve probably heard the rumors. You might have seen posts online claiming it ruins your gut, steals your energy, or causes rare but deadly complications. So, why do some people say metformin is bad to take?
The short answer is: it isn’t “bad” for everyone. For millions, it’s a life-saving tool that prevents blindness, kidney failure, and heart disease. However, it does come with real, documented downsides. These aren’t just myths; they are physiological reactions that affect a significant number of users. If you’re struggling with nausea, fatigue, or digestive issues, you’re not imagining things. Let’s look at exactly what goes wrong for some people and how to tell if the risks outweigh the benefits for you.
The Gut Troubles: Why Your Stomach Hates Metformin
If there is one complaint louder than any other, it’s gastrointestinal distress. Up to 30% of people who start taking this drug report stomach issues. This isn’t a minor inconvenience for many; it can be debilitating. You might experience diarrhea, bloating, gas, or a general feeling of nausea shortly after eating.
Why does this happen? Metformin changes the way your gut bacteria behave. Recent studies show it alters the microbiome composition, increasing certain types of bacteria that produce more gas and short-chain fatty acids. While these fatty acids can actually help lower blood sugar, the gas production leads to that uncomfortable bloated feeling. Additionally, the drug slows down gastric emptying, meaning food sits in your stomach longer, which can trigger nausea.
| Symptom | Frequency | Typical Onset | Duration |
|---|---|---|---|
| Diarrhea | ~20-30% | First few days | Often resolves in weeks |
| Bloating/Gas | ~15-25% | Within first week | Can persist long-term |
| Nausea | ~10-15% | Immediate | Usually temporary |
| Loss of Appetite | ~10% | Variable | May aid weight loss |
For many, these symptoms fade as the body adjusts. Doctors often recommend starting with a low dose and slowly increasing it. Taking the extended-release version (ER) also helps because it releases the drug slowly into your system, reducing the shock to your gut. But for some, the discomfort never fully goes away, making daily life unpleasant.
The Silent Thief: Vitamin B12 Deficiency
This is perhaps the most under-discussed downside. Long-term use of metformin interferes with the absorption of Vitamin B12 in your ileum (the last part of your small intestine). It doesn’t matter if you eat plenty of meat or dairy; the drug blocks the uptake mechanism.
Studies suggest that up to 30% of patients on long-term metformin therapy develop clinically significant B12 deficiency. Why is this bad? B12 is crucial for nerve health and red blood cell formation. A deficiency can lead to:
- Pernicious anemia: Fatigue, weakness, and pale skin.
- Neuropathy: Tingling, numbness, or pain in hands and feet. This is tricky because diabetic neuropathy already causes similar symptoms, so the drug-induced deficiency can worsen existing nerve damage without anyone realizing it.
- Cognitive decline: Memory issues and brain fog.
The fix is simple-B12 supplements-but only if you know to check your levels. Many people suffer from fatigue and assume it’s just “aging” or “diabetes,” when it’s actually their medication causing a nutrient gap. Regular blood tests are essential if you’re on this drug.
Lactic Acidosis: The Rare but Serious Risk
You’ll see warnings about lactic acidosis on every bottle. It sounds scary because it is. Lactic acidosis occurs when lactate builds up in your bloodstream faster than your body can remove it. This makes your blood acidic, which can stop your organs from functioning properly. It has a high mortality rate if not treated immediately.
However, here is the context: this event is incredibly rare. In healthy individuals with normal kidney function, the risk is negligible-less than 1 case per 100,000 patient-years. The danger spikes significantly if you have specific risk factors:
- Kidney impairment: If your kidneys can’t filter the drug out, it accumulates.
- Heart failure: Poor circulation reduces oxygen delivery, promoting lactate production.
- Excessive alcohol consumption: Alcohol metabolism increases lactate levels.
- Severe infections or dehydration: These stressors can trigger metabolic shifts.
If you have healthy kidneys and don’t abuse alcohol, this risk is theoretical for you. But if you have chronic kidney disease (CKD), doctors will monitor your eGFR (estimated glomerular filtration rate) closely. If it drops below 45 mL/min/1.73 m², they may reduce the dose. Below 30, they usually stop the drug entirely.
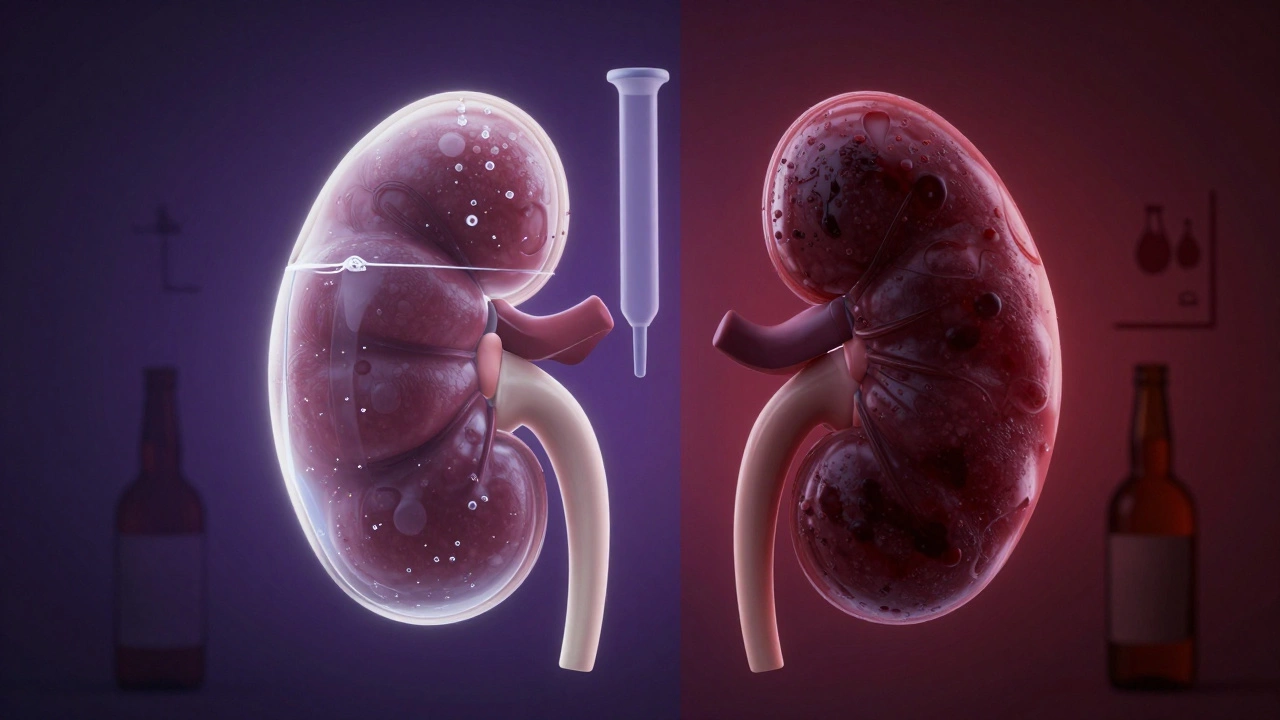
Hepatic Concerns and Liver Health
There is ongoing debate about whether metformin affects the liver. Some older studies suggested potential hepatotoxicity, but modern consensus says it’s generally safe for the liver. In fact, it’s often beneficial for people with Non-Alcoholic Fatty Liver Disease (NAFLD) because it improves insulin sensitivity, which helps reduce fat accumulation in the liver.
However, caution is advised if you have severe liver disease. Since the liver plays a role in metabolizing lactate, impaired liver function could theoretically increase the risk of lactic acidosis. Most guidelines say avoid it in cases of active hepatitis or cirrhosis, but mild liver enzyme elevations are usually not a contraindication.
Weight Loss: A Side Effect or a Benefit?
Some people complain that metformin makes them feel “too thin” or causes unwanted weight loss. Others love it for this reason. Unlike some other diabetes drugs like sulfonylureas or insulin, which cause weight gain, metformin is weight-neutral or slightly weight-reducing.
It works by decreasing glucose production in the liver and improving insulin sensitivity. It also slightly reduces calorie absorption in the gut. For someone trying to manage both diabetes and obesity, this is a huge plus. But for someone who is already underweight or frail, this unintended weight loss can be concerning. It can lead to muscle wasting if not monitored with proper nutrition.
Who Should Avoid Metformin?
Understanding who should *not* take this drug is just as important as knowing its side effects. You should likely avoid it or seek alternatives if:
- You have an eGFR below 30 mL/min/1.73 m².
- You have a history of lactic acidosis.
- You have severe heart failure or hypoxic states.
- You consume large amounts of alcohol regularly.
- You are scheduled for procedures involving iodinated contrast dye (you may need to pause the drug temporarily).
If you fall into any of these categories, talk to your doctor about alternatives like GLP-1 receptor agonists (e.g., semaglutide) or SGLT2 inhibitors (e.g., empagliflozin), which work differently and may have different side effect profiles.
Does metformin damage your kidneys permanently?
No, metformin does not damage your kidneys directly. In fact, it may offer some protective benefits against diabetic nephropathy. However, if your kidneys are already damaged, they cannot filter the drug effectively, leading to toxic buildup. This is why doctors test your kidney function before prescribing it and monitor it regularly.
Can I take metformin if I drink alcohol occasionally?
Occasional moderate drinking is generally considered safe for most people on metformin. However, heavy or binge drinking significantly increases the risk of lactic acidosis and hypoglycemia (low blood sugar), especially if you skip meals. It’s best to limit intake and discuss your habits with your healthcare provider.
How do I fix metformin-induced B12 deficiency?
The most effective way is through supplementation. Oral B12 tablets or sublingual lozenges work well, though some people prefer injections for faster results. Ask your doctor to check your serum B12 levels annually. If deficient, they will prescribe a specific dosage based on your blood work.
Is extended-release metformin better than immediate-release?
For many people, yes. Extended-release (ER) metformin dissolves slowly in the gut, which drastically reduces gastrointestinal side effects like diarrhea and bloating. It also allows for once-daily dosing, which improves adherence. If immediate-release causes stomach upset, switching to ER is often the first step doctors recommend.
What are the best alternatives to metformin?
If you cannot tolerate metformin, common alternatives include SGLT2 inhibitors (like Jardiance or Farxiga), which help excrete sugar through urine, and GLP-1 receptor agonists (like Ozempic or Trulicity), which improve insulin secretion and slow digestion. Sulfonylureas are another option but carry a higher risk of weight gain and hypoglycemia.