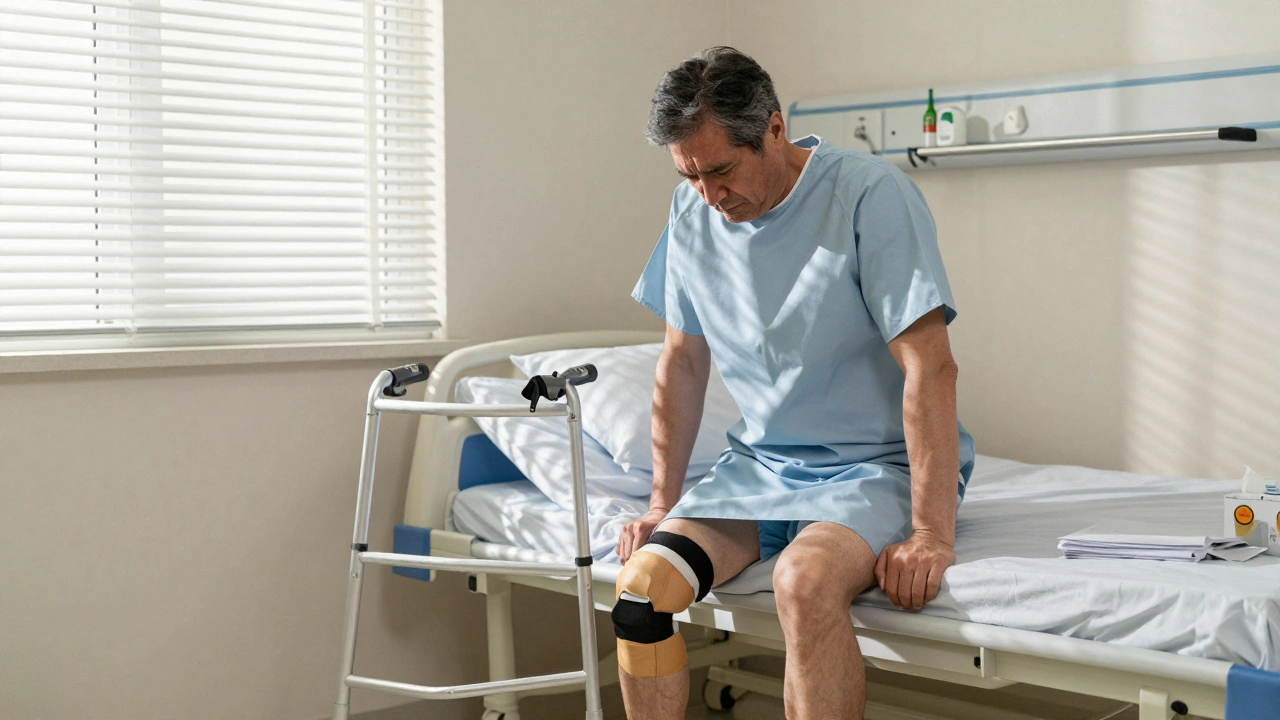
After knee replacement surgery, most people expect to feel better. And they do - eventually. But the road there? It’s not what most patients prepare for. The hardest part of knee replacement recovery isn’t the surgery itself. It’s not even the first few days in pain. It’s the loss of mobility and the long, frustrating grind to get it back.
The Silent Struggle: Losing Your Independence
You walk into the hospital with a bad knee. You walk out with a new one. Sounds simple, right? But in the weeks that follow, your body doesn’t cooperate. You can’t bend your leg fully. You can’t stand up without help. You can’t climb stairs. Even simple things like getting out of bed or stepping into the shower become battles. This isn’t just physical - it’s emotional. People don’t talk about how hard it is to feel like a child again, needing help to do the things you once took for granted.
Studies show that over 60% of patients report significant difficulty with daily tasks three weeks after surgery. By six weeks, that number drops to around 35%. But those first six weeks? They’re brutal. You’re not just healing. You’re relearning how to move.
Pain Isn’t the Worst Part - Stiffness Is
Yes, pain is real. But it’s usually managed with medication. The real problem is stiffness. Your new knee joint doesn’t just snap into place. It’s surrounded by scar tissue, swollen muscles, and tight tendons. That’s why you can’t get your knee to bend past 90 degrees - even though your surgeon says it should be 110.
Many patients give up on physical therapy because it hurts. They think, “If it hurts this much, I’m doing damage.” But that’s not true. The burning sensation during stretching? That’s your body adapting. It’s not injury. It’s progress. The key is consistency, not intensity. One patient in Bangalore, 72, told me he did his stretches every morning before coffee - even on days he felt like quitting. By week eight, he walked to the park alone. That’s the difference.
Physical Therapy: The Make-or-Break Factor
Here’s the truth: if you skip physical therapy, you’ll never fully recover. No surgeon can fix a stiff knee alone. No pill can loosen scar tissue. Only movement can.
But not all therapy is created equal. Some clinics just hand you a sheet of exercises and say, “Do these.” That’s not enough. Effective therapy includes:
- Manual mobilization - a therapist gently moves your knee to break up adhesions
- Heat and cold therapy to reduce swelling
- Progressive resistance training, starting with ankle weights
- Balance drills to rebuild confidence
Patients who stick with a structured program for at least 12 weeks are three times more likely to regain full range of motion than those who stop early. And yes, it’s tiring. It’s boring. It’s hard to stay motivated. But your knee doesn’t care how you feel. It only responds to repetition.
The Mental Toll Nobody Warns You About
Recovery isn’t just physical. It’s psychological. You wake up every morning hoping today will be better. Some days it is. Other days, your knee feels worse than the day after surgery. That’s normal. But it’s also exhausting.
Depression and anxiety are common after joint replacement. One 2024 study from the Journal of Orthopaedic Research found that 42% of patients showed signs of mild to moderate depression in the first two months. Why? Because they feel trapped. They can’t work. They can’t socialize. They feel useless.
The fix? Not medication. It’s connection. Talking to someone who’s been through it. Joining a support group. Even texting a friend once a day. Small wins matter. Did you walk to the mailbox? That’s a win. Did you do your stretches without crying? That’s a win too.
Why Some People Never Fully Recover
Not everyone gets back to normal. Why? Three reasons:
- They quit too soon. Most people stop therapy at six weeks. That’s when the pain fades - but the stiffness remains.
- They don’t follow the home program. Therapy sessions are once or twice a week. The real work happens at home.
- They ignore swelling. Swelling is the enemy of motion. Ice it. Elevate it. Don’t ignore it.
Patients who return to normal function after a year almost always share one habit: they never skipped a day of movement. Not even for a holiday. Not even when they were tired.
What Actually Works: Real Strategies from Real Patients
Here’s what helps - not what sounds good, but what works:
- Use a stationary bike. It’s low-impact, builds range, and feels good. Start with 5 minutes a day. Increase by 1 minute every 3 days.
- Walk barefoot on grass. It improves balance and strengthens foot muscles that support your knee.
- Ice for 20 minutes after activity. Swelling is what locks your joint. Ice reduces it. Simple.
- Track your progress. Write down your knee bend angle each week. Even a 2-degree gain is progress.
One woman in Hyderabad, 68, started with 70 degrees of bend. After 10 weeks of daily biking and stretching, she hit 115. She now hikes with her grandchildren. She didn’t have magic therapy. She just showed up.

The Timeline You Need to Know
Recovery isn’t linear. But here’s what to expect:
- Week 1-2: Pain, swelling, dependence on walkers or crutches.
- Week 3-6: Stiffness peaks. This is the hardest phase. Most people quit here.
- Week 7-12: Mobility improves rapidly. You start walking without help.
- Month 4-6: Strength returns. You can climb stairs, drive, and sleep on your side.
- Month 12: Full recovery. Most patients report better function than before surgery.
Don’t compare your week 4 to someone else’s week 12. Everyone heals differently. Your job is to show up - not to be perfect.
When to Worry (And When Not To)
Some things are normal. Some aren’t.
Normal:
- Mild swelling for up to 3 months
- Clicking or popping sounds
- Warmth around the joint
- Temporary numbness on the outer thigh
Call your doctor if:
- Fever over 101°F (38.3°C)
- Redness spreading around the incision
- Sudden, severe pain
- Calf pain or swelling (could be a blood clot)
Most discomfort is part of healing. But don’t ignore warning signs.
Final Thought: It’s a Marathon, Not a Sprint
The hardest part of knee replacement recovery isn’t the pain. It’s the waiting. It’s the doubt. It’s the feeling that you’ll never be the same. But you will. Not because of surgery. Because of you. Because you showed up. Because you stretched when you didn’t want to. Because you didn’t give up.
It’s not about being strong. It’s about being consistent.
How long does it take to walk normally after knee replacement?
Most people can walk without assistance by 6 to 8 weeks. But walking normally - with full stride, no limp, no pain - usually takes 3 to 6 months. Full recovery, including strength and confidence, can take up to a year.
Why is my knee still stiff 3 months after surgery?
Stiffness at 3 months is common, especially if you haven’t been consistent with physical therapy. Scar tissue and muscle tightness can linger. The good news? It’s still reversible. Daily stretching, heat therapy, and low-impact movement like cycling can improve flexibility even at this stage. Talk to your therapist - don’t assume it’s permanent.
Can I overdo physical therapy after knee replacement?
Yes - but not in the way most people think. You can’t “overwork” your knee by stretching. But you can push too hard too fast, leading to swelling and setbacks. The key is consistency, not intensity. Do your exercises daily, even if only for 10 minutes. Better to do a little every day than one long, painful session once a week.
Is it normal to have pain at night after knee replacement?
Yes, especially in the first few months. At night, there’s less movement and more swelling. Your body also processes inflammation differently while resting. Use ice before bed, elevate your leg, and avoid sleeping on your stomach. If pain wakes you up regularly after 3 months, check with your doctor - it could signal an issue like infection or implant misalignment.
Do I need to do therapy for life after knee replacement?
No, but staying active is. You don’t need formal therapy forever. But you do need to keep moving. Walking, swimming, cycling, and light strength training should become lifelong habits. A knee replacement lasts 15-20 years - but only if you take care of it. Think of it like a car: regular maintenance keeps it running.