IVF Process Interactive Roadmap
Click on a stage below to explore the details of each phase of the IVF journey.
Ovarian Stimulation
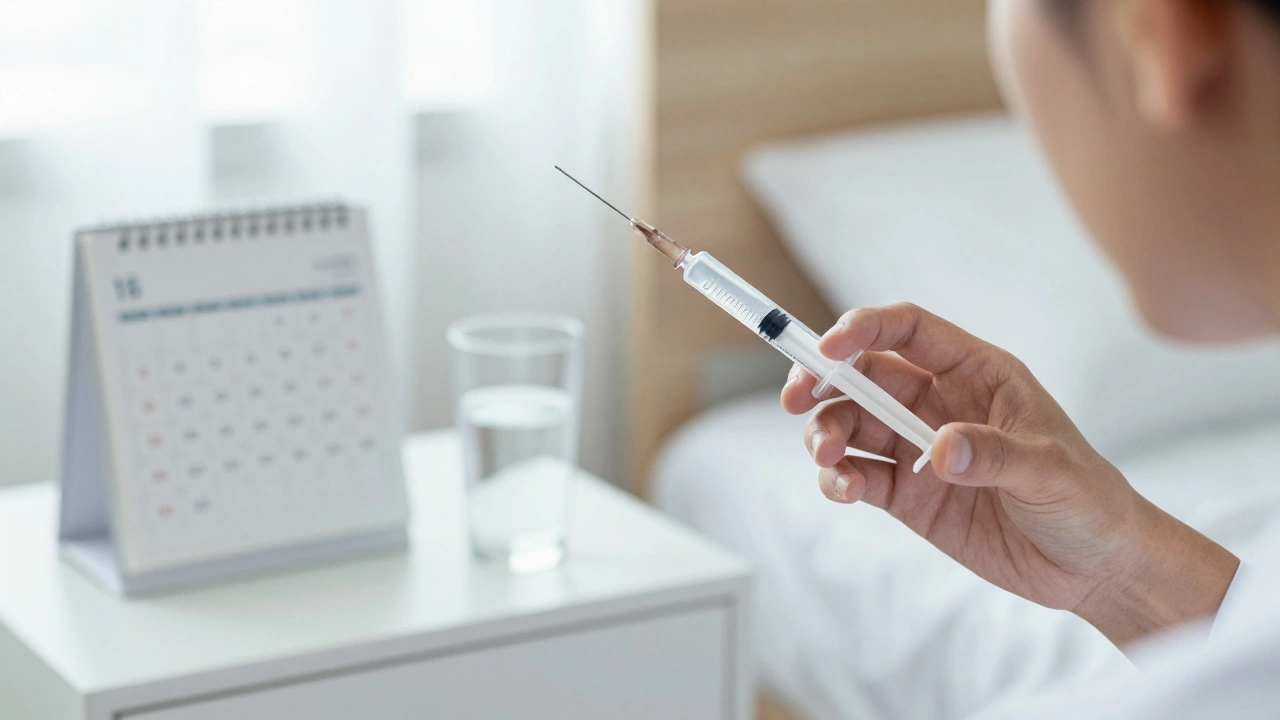
Injectable hormones (FSH/hMG) are used to stimulate the ovaries to produce multiple eggs instead of just one.
- Frequent ultrasounds and blood tests (monitoring)
- Ends with a "trigger shot" to finalize maturation
- Typically lasts 8 to 14 days
Egg Retrieval
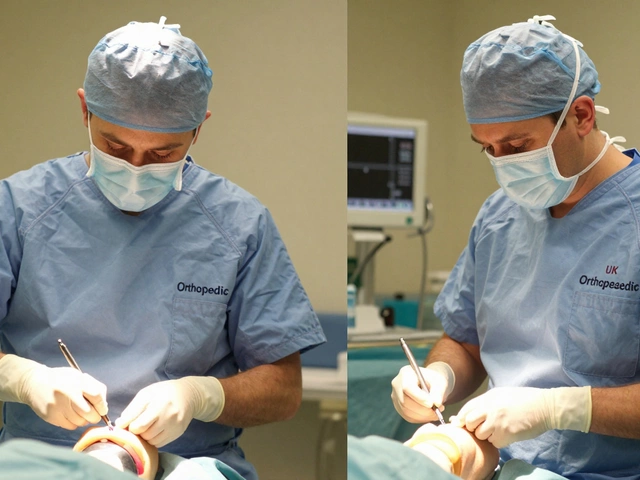
A minor surgical procedure using a needle to aspirate follicles from the ovaries under ultrasound guidance.
- Performed under sedation or general anesthesia
- Takes 20 to 40 minutes
- Occurs 34-36 hours after the trigger shot
Fertilization
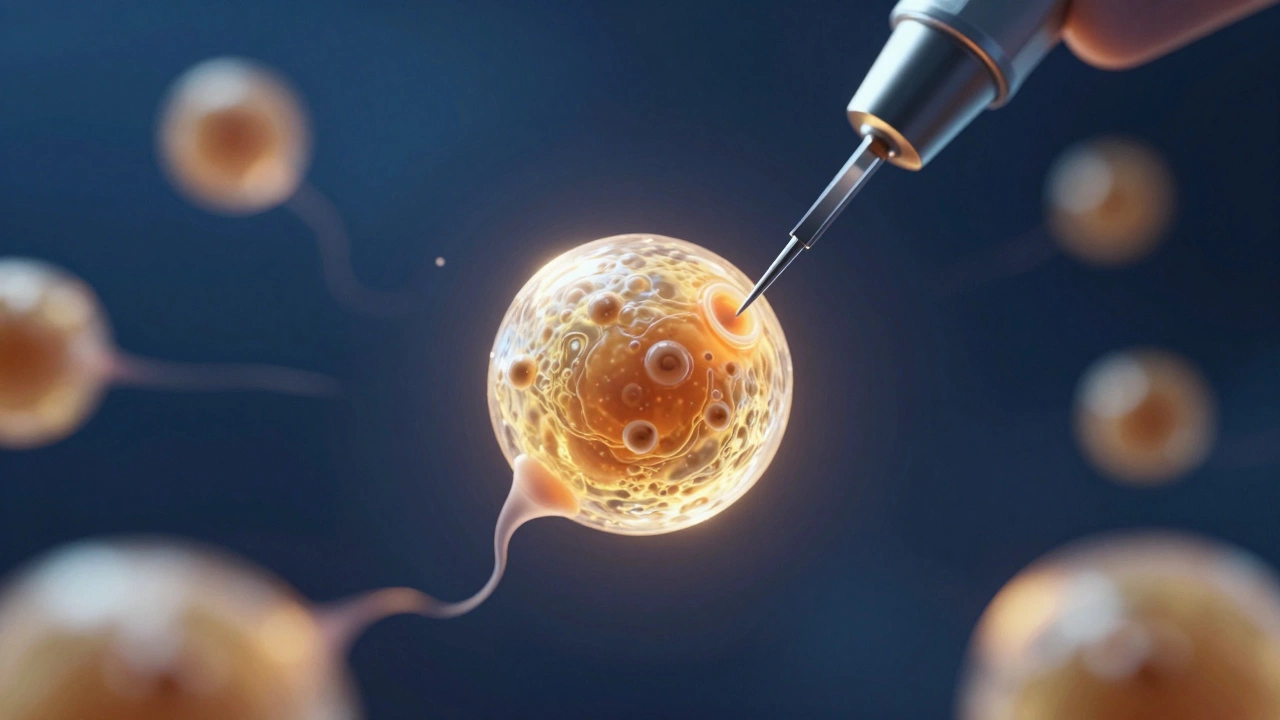
Eggs are joined with sperm in the lab via conventional insemination or ICSI (Intracytoplasmic Sperm Injection).
- Embryologists check for two nuclei (proof of fertilization) the next morning
- Determines how many embryos will proceed to growth
Embryo Culture
Embryos grow in a high-tech incubator. Most clinics aim for the Blastocyst stage (Day 5 or 6).
- Day 3: Cleavage stage (6-8 cells)
- Day 5-6: Blastocyst stage (Higher implantation rate)
Embryo Transfer
The embryo is placed into the uterus via a thin catheter. Can be a "fresh" or "frozen" transfer.
- Similar to a pap smear (usually no anesthesia)
- Frozen transfers allow the body to recover from hormones
- Full bladder helps ultrasound visibility
Quick Takeaways
- IVF consists of five main phases: stimulation, retrieval, fertilization, growth, and transfer.
- The timeline usually spans one full menstrual cycle, though some people opt for "freezing" embryos to recover physically.
- Success depends on factors like age, egg quality, and the specific protocol used by the clinic.
- Preparation and mental health support are as vital as the medical procedures themselves.
Getting Ready and the First Stage: Ovarian Stimulation
Before the actual 5 stages of IVF begin, you usually start with a baseline appointment. Your doctor checks your ovaries via ultrasound to see how many follicles (the small sacs that hold eggs) are present. Once you're cleared to start, the first official stage is Ovarian Stimulation is the process of using injectable hormones to stimulate the ovaries to produce multiple eggs instead of the single egg usually released during a normal cycle.
In a typical month, your body picks one dominant follicle. In IVF, we want more. Why? Because not every egg retrieved will be mature, and not every fertilized egg will become a healthy embryo. By producing a group of eggs, you increase your statistical chances of success. You'll likely use medications like FSH (Follicle Stimulating Hormone) or hMG (human Menopausal Gonadotropin) for about 8 to 14 days.
During this time, you'll be a regular at the clinic for "monitoring." This involves frequent blood tests and ultrasounds to track follicle growth. If the follicles grow too quickly, your doctor might adjust your dose. The goal is to hit the "sweet spot"-large enough to be mature, but not so large that they rupture prematurely. This stage ends with a "trigger shot," usually hCG or a Lupron trigger, which tells the eggs to finish maturing over the next 36 hours.
Stage Two: Egg Retrieval
Once the trigger shot is administered, the clock starts. You cannot miss the window for Egg Retrieval is a minor surgical procedure where a needle is used to aspirate follicles from the ovaries under ultrasound guidance. This usually happens about 34 to 36 hours after the trigger.
You'll be under light sedation or general anesthesia, so you won't feel the needle. The doctor uses an ultrasound probe to see the follicles and a thin needle to suction the fluid-and the egg-out of each one. The whole thing takes about 20 to 40 minutes. While you're napping, the embryologist is in the next room, searching through the fluid under a microscope to find the eggs.
Recovery from retrieval is usually quick, but you might feel bloated or have mild cramping. It's common to feel like you've just had a heavy workout. Pro tip: have a heating pad and plenty of electrolyte drinks ready at home. This is the most physically demanding part of the process for the woman, and resting for 24 hours is non-negotiable.
Stage Three: Fertilization and the Lab Work
Now the focus shifts from the patient to the lab. This is where Fertilization happens. The clinic uses the partner's sperm (collected on the day of retrieval) or donor sperm to join with the eggs. There are two main ways this happens: conventional insemination and ICSI.
ICSI (Intracytoplasmic Sperm Injection) is a technique where a single, healthy sperm is injected directly into a mature egg. This is often used if there are concerns about sperm count or motility, or if previous IVF attempts had low fertilization rates. It removes the guesswork and ensures the sperm actually makes it inside the egg.
The next morning, the embryologist checks for "fertilization." They look for two pronouns (nuclei) in the cell, which proves the sperm and egg have merged. This is often the most nerve-wracking phone call of the whole process. You'll find out how many eggs were mature, how many fertilized, and how many are now officially embryos.
| Feature | Conventional Insemination | ICSI (Sperm Injection) |
|---|---|---|
| Method | Sperm and eggs placed in a dish together | Single sperm injected into the egg |
| Best For | Normal sperm parameters | Male factor infertility or low sperm count |
| Control | Natural selection of sperm | Embryologist selects the best sperm |
| Success Rate | High for compatible pairs | Generally higher for severe male infertility |
Stage Four: Embryo Culture and Development
Fertilized eggs don't just stay as single cells. They begin to divide. For the next 3 to 6 days, the embryos live in a high-tech incubator that mimics the environment of the human body. This is the Embryo Culture phase.
Initially, the embryo is a "cleavage stage" embryo (Day 3), consisting of about 6 to 8 cells. However, most clinics now prefer to grow embryos to the Blastocyst stage. A blastocyst is an embryo that has reached Day 5 or 6 and has developed a fluid-filled cavity. Blastocysts have a much higher chance of successful implantation in the uterus than Day 3 embryos.
During this window, some people choose PGT-A (Preimplantation Genetic Testing for Aneuploidies). This involves taking a few cells from the outer layer of the blastocyst to check for chromosomal abnormalities. For example, it can detect if an embryo has an extra copy of chromosome 21 (Down Syndrome). This helps doctors pick the healthiest embryo for transfer, reducing the risk of miscarriage.
Stage Five: The Embryo Transfer
The finale is the Embryo Transfer, where the embryo is placed into the uterus. This can happen in a "fresh cycle" (right after retrieval) or a "frozen cycle" (where the embryo is thawed and transferred later). Many doctors now recommend frozen transfers because it gives the woman's body time to recover from the hormone surges of the stimulation phase, potentially creating a more receptive uterine lining.
The procedure itself is simple. A thin catheter is inserted through the cervix, and the embryo-suspended in a tiny drop of fluid-is gently placed into the uterine cavity. It's similar to a pap smear and usually doesn't require anesthesia. You'll likely be asked to hold your bladder full, as this helps the doctor see the uterus better on the ultrasound.
After the transfer, you enter the "two-week wait." This is the gap between the transfer and the pregnancy test. While you might be tempted to buy a home test immediately, remember that IVF medications (like progesterone) can cause a false positive. Waiting for the official blood test (beta-hCG) is the only way to get a definitive answer.

Common Hurdles and How to Handle Them
Not every IVF cycle goes perfectly. Sometimes you might experience OHSS (Ovarian Hyperstimulation Syndrome), where the ovaries overreact to the meds, causing bloating and pain. This is why monitoring is so critical; doctors can "coast" your dosage or use a specific trigger to prevent it.
Another common issue is a "failed cycle," where no embryos develop or none implant. This doesn't always mean you can't have a baby; it often means the protocol needs a tweak. Maybe you need a different medication or a different timing for the transfer. Many people succeed on their second or third attempt, not the first.
Managing the mental load is just as important as the physical side. The 5 stages of IVF are a marathon, not a sprint. Whether it's through a support group or a specialized fertility counselor, talking about the anxiety of the "two-week wait" can make the process feel less isolating.
How long does the entire IVF process take?
A single IVF cycle typically takes about 4 to 6 weeks from the start of stimulation to the pregnancy test. However, if you choose to freeze your embryos and do a frozen embryo transfer (FET), the process can stretch over several months to allow your body to recover.
Is egg retrieval painful?
Because the procedure is performed under sedation or general anesthesia, you won't feel pain during the actual retrieval. Most people experience mild cramping, bloating, and soreness for a few days afterward, similar to menstrual cramps.
What is the difference between a Day 3 and Day 5 embryo?
A Day 3 embryo is at the cleavage stage (about 6-8 cells), while a Day 5 embryo is a blastocyst. Blastocysts are more developed and generally have a higher implantation rate, which is why many clinics prefer to wait until Day 5 before transferring.
Do I have to do genetic testing (PGT-A) on my embryos?
No, PGT-A is optional. It is highly recommended for women over 35 or those with a history of recurrent miscarriages, as it identifies embryos with the correct number of chromosomes. However, some choose to skip it due to the cost or the risk of losing a potentially viable embryo during the biopsy.
What happens if no embryos are suitable for transfer?
If no viable embryos are created, your doctor will analyze the cycle to see where things went wrong. They may change the stimulation drugs, adjust the dosage, or suggest alternative options like using donor eggs or sperm for the next attempt.
Next Steps and Troubleshooting
If you're just starting, your first step is to find a Reproductive Endocrinologist (RE) you trust. Ask them about their success rates for your specific age group and their philosophy on "fresh vs. frozen" transfers. If you've already gone through a cycle that didn't work, request a full review of the lab reports-specifically the fertilization rate and the embryo grading.
For those currently in the stimulation phase: keep a log of your symptoms and medication times. Small details, like how you felt after the trigger shot, can help your doctor refine the process for future cycles. If you experience severe shortness of breath or extreme abdominal pain during stimulation, contact your clinic immediately, as these can be signs of OHSS.